

Country-led innovations for treating childhood diabetes
Presented by Novo Nordisk

Diabetes in children is a rising problem in developing countries.
But, there are reasons to be positive that progress is being made.
The International Diabetes Federation (IDF) estimates that in total there are more than 1.1 million children and adolescents living with type 1 diabetes globally. The greatest rise in diabetes prevalence is projected to occur in Africa, but the continent spends the least on diabetes care as a proportion of global annual healthcare spending.
While that picture is cause for concern, some developing nations are working on improving access to care and medicine in partnership with the Changing Diabetes in Children (CDIC) programme. The partnership has been running since 2009, supporting patient education, healthcare professionals’ training and clinic improvements. The number of children with diabetes reached surpassed 29,000 in 18 countries in 2021, but the aim is to reach 100,000 by 2030.
The IDF’s estimate of 1.1 million children might be conservative. In four of the 18 countries in which the CDIC runs (Guinea, the Democratic Republic of Congo, Kenya and Ethiopia) more children were diagnosed with diabetes and enrolled in the programme than the IDF estimated have the disease.

Calculating and addressing the increasing burden of diabetes will require a multifaceted approach. Training healthcare professionals, educating patients, improving clinics and access to insulin are all made more possible with technologies like telemedicine and digital records. But to reach a stage where those technologies are effective, developing nations have other hurdles to climb first.
Why does type 1 diabetes, a disease we have been able to treat for a century, remain a problem in so many developing countries?
Each vial leaves the factory labelled in its destination’s language, packaged in insulated boxes, stacked up on a pallet and connected to a temperature-monitoring device. Should the temperature of these boxes of vials deviate from 2-8ºC at any point, the consignee will know.
Vials from factories with the correct licenses in their country of origin have “known consignor” status at the airport, meaning they whizz through the airport security. At this point, some of the pallets are broken up by a European distributor in Belgium who might have an eye out for countries who are not well set up to take a whole pallet of insulin.
Smaller countries might demand far fewer vials than an entire pallet in a year. In Guinea Bissau, a country of two million people around 3,000km (1,864 miles) along Africa’s west coast from Ghana, wholesalers can make a living by selling 20 vials at a time to local pharmacies. Their annual demand is never high enough to warrant flying in a shipment.
Ghana, with a population of over 30 million, is large enough to take a pallet-load. But, that doesn’t mean that wholesalers are skipped completely.
Procurement
It can take up to eight weeks for insulin to reach this point.
When the shipment lands in Ghana it is first taken on a trolley, wrapped in its thermal blanket, into cold storage at the airport, where the temperature logger is checked to ensure the product has remained cool on its flight. It’s then up to the consignee to clear the product through customs. If the vials have been too hot, they will not be cleared. If the consignee is a wholesaler, the first markups (which could be import duties taxes and tariffs) are applied, currencies are converted and the cost of the vials goes up.
Procurers in Ghana tell Novo Nordisk how much they would like to purchase to use over several months, and the vials are shipped in one batch. Accurate forecasting is essential, particularly for countries like Ghana that are working with tight margins for error. The capacity to take a large shipment and then distribute it to small, regional clinics is much more limited in Ghana than, say, Europe. “When you get all of it in one go, your ability to store it becomes harder,” says Prashant Yadav, a senior fellow at the Center for Global Development, whose work focuses on improving healthcare supply chains.

To speed up the process, Ghana avoids storing large quantities of insulin centrally in the public health system, instead choosing to distribute the insulin regionally. “As part of our strategy to remove some barriers to access, we contract suppliers to deliver agreed quantities of commodities to our regional warehouses,” says Joycelyn Azeez, a director of pharmaceutical services at the Ghanaian Ministry of Health. “So even though the tender is processed centrally by a multidisciplinary team including representatives of the regional pharmacists, the actual contracts are between the suppliers and the various Regional Health Administrations.”
Many clinics are severely understaffed, says Yadav. Their staff might amount to a nurse, pharmacy technician, admin officer and cleaner. So it may be difficult to obtain accurate forecasting from already stretched staff who are not trained in supply chains.
In Ghana demand is intrinsically uncertain. When clinics and their patients are so remote, about 43% of Ghanaians live rurally, there is a lot that can mean a patient misses their prescription.

Furthermore, in Ghana not everyone goes to a government-run clinic. “Around 50% are going to private clinics or private hospitals,” says Yadav, and more still seek treatments from faith groups.
“The structure of the health system in Ghana is such that there are different agencies under the Ministry of Health. For example, the Ghana Health Service, Tertiary Hospitals, Christian Health Association Of Ghana,” says Priscilla Addison, a doctor at Our Lady of Grace Hospital, Ghana.
Addison says that working for an independent healthcare facility like those run by the Christian Health Association of Ghana poses its own procurement problems. “Typically, hospitals procure insulin with their funds and are later reimbursed by the government,” she says. “However, there's usually a delay in the reimbursement so hospital management may decide not to buy certain drugs, for example insulin. In such cases, patients usually have to search for the medications at private pharmacies and in rural areas this poses a huge challenge.”
Some patients who use the private market are subject to other problems. “Between the manufacturer and the private clinic there are wholesalers, sub-wholesalers, sub-sub-wholesalers and each includes their markup,” says Yadav. “People could be paying a more than 100% markup. For some people these drugs are unaffordable, but adding 100% on top makes it certainly unaffordable.” The reliance on private distributors ultimately hits patients in their pocket.
But, “there is a new distribution system in place in Ghana that uses third-party logistics to distribute medicines from the regional warehouses to the health facilities,” says Azeez. “Under this arrangement, requisitions are made from the facilities to the regional warehouses electronically, the requisitions are processed and the third-parties transport the insulin to the various warehouses,” which simplifies the process, she says.
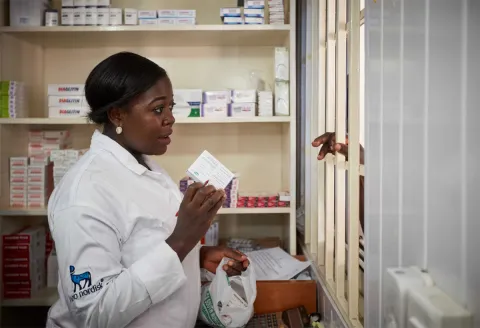
When the delivery is finally made to the clinic, the trucks are unloaded and vials placed in fridges. After an arduous journey, they arrive still within that temperature sweet spot. Now, it’s up to the clinic to distribute it to their patients.
Yadav says that if deliveries to remote locations can be made more regularly, and sustainably, tech can make the job of forecasting easier.
“Every healthcare worker who has to order drugs can be given a relatively inexpensive phone or tablet and that allows them to enter what was used last month or last week,” says Yadav. He believes that eventually, with enough data, artificial intelligence might be better able to make predictions on behalf of healthcare staff if demand could be tracked accurately. Would the central government stand a better chance of forecasting?
Could some of the fridges currently used to store vaccines be repurposed to store a small quantity of insulin, too, he asks?
Perhaps there are ways to avoid the most difficult parts of the route? Where infrastructure is poor, could drones be used for small quantities of drugs over short distances?

What matters most to the patient is that they receive the right care in a timely fashion. For Mousakas, a young teacher from Breman Brakwa, a farming community in the central region of Ghana, the diagnosis of diabetes came as a shock – something that is seen as only affecting the wealthy in Africa. Mousakas was originally prescribed another medication and only had access to insulin after it became available at the Our Lady of Grace hospital. Without that intervention, teaching might have become impossible.
Mousakas’s story is not isolated. Patients must be prescribed insulin to receive it, which requires doctors with specialist training to make the right diagnosis and prescription, to which there is limited access in Ghana.
The whole journey has taken months and has not been without its challenges. Ultimately, whether a patient is able to access insulin is down to a lot of factors, not least the affordability of the final product, stockouts and delays.
For now our vial has served its purpose, its precious contents have helped to better the life of another patient. But it’s easy to see a future in which insulin fridges are powered by mobile phone masts, vials flown in by drone and data is seamlessly synchronised across the cloud. In that future its journey might have been made a little bit easier.
This work has been made possible thanks to Novo Nordisk.