Fiji hikes health taxes and adopts guidelines to tackle NCDs, which consume 40% of healthcare costs

Fiji has increased taxes on sugary drinks, other processed foods, alcohol and tobacco in its new budget. This comes as a Ministry of Health (MoH) official says the effects of noncommunicable diseases (NCDs), cost the country US$ 591.41 million a year.
The taxes imposed by the Western Pacific island country include hiking the domestic excise tax from 35 to 40 cents per kilogram or per litre on juice, ice cream, sweet biscuits, snacks, and sugar confectionery, and introducing an import excise of 15% on those items; and raising excise taxes on tobacco and alcohol by 5%.

Unhealthy foods, tobacco and alcohol are major risk factors for NCDs, which cause 74% of death and disability globally, hitting low- and middle-income countries the hardest. NCDs include cancers, cardiovascular disease, stroke, chronic respiratory diseases, diabetes, mental health and neurological conditions and chronic kidney disease, amongst others.
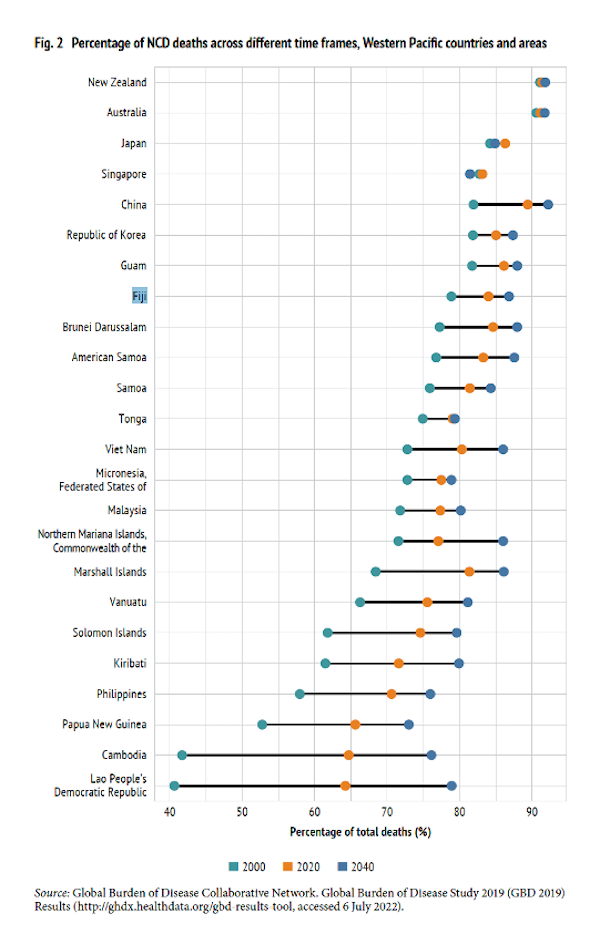
In 2019, 87% of deaths in the Western Pacific region were caused by NCDs, with high rates of premature death (before the age of 70). In Fiji, diabetes alone causes one-fourth of all deaths, or about 1500 per year, the highest rate in the world. This is attributed in large part to a shift towards higher consumption of imported ultra-processed foods, and away from traditional diets based on fresh fish and produce. The human right to healthy food was included in the country’s constitution in 2013, as traditional diets are threatened in Fiji and many other small island developing states (SIDS) by both the ultra-processed food industry and climate change.
When announcing the taxes, Deputy Prime Minister and Finance Minister Biman Prasad noted that alcohol taxes had been cut by 50% during the COVID-19 pandemic. “We are mindful that alcoholic beverages are an integral part of our tourism industry... so we are starting with a very small increase compared to the massive reduction we had two years ago.”
MoH Head of Wellness, Dr Devina Nand, said that NCDs represent 40% of all health spending in Fiji. “The direct cost burden of NCDs is greater than the direct cost burden of infectious diseases combined with reproductive health and malnutrition,” she added at the launch of new NCD guidelines for primary healthcare centres.
The guidelines will save money and improve care by standardizing the approach to NCDs care, said Nand. They’re known as the Cardiovascular Risk Assessment and Management (CRAM)/ Package of Essential Noncommunicable (PEN) Operational Guidelines for Fiji’s Primary Health Care Facilities.
“The Fiji CRAM will help to improve the coverage of appropriate, ethical, quality and standardised service for people living with NCDs," said Nand, quoted in The Fiji Times newspaper. “It harnesses an integrated approach for effective interventions in low-resource settings, allowing efficient use of limited resources.”
The budget’s tax increase comes just weeks after a SIDS conference, where countries including Fiji adopted the Bridgetown Declaration. It addresses the commercial determinants of health and climate change as the main drivers of the burden of NCDs in SIDS, and outlines a SIDS-specific approach to address them.
“Despite our best efforts, our progress on NCD prevention and control is slow and patchy,” said Sir Collin Tukuitonga, co-chair of the SIDS High-Level Policy Expert Group. “Most SIDS will not achieve agreed NCD targets. Clearly, we need to do more, do better things, do things better and do so with urgency.”
“The Bridgetown Declaration is an excellent opportunity to accelerate our actions on NCD prevention and control,” he continued. “Several possible actions are provided to be implemented appropriate to local circumstances. I encourage SIDS to take action.”
WHO’s recently released Regional action framework for noncommunicable disease prevention and control in the Western Pacific calls for transforming “sick systems” — in which unhealthy environments add to the NCD burden and the health sector is reactive and treatment focused — into “health systems” where societies invest in health-enabling environments and the health sector supports life-long individual health and wellness.
“Actions to prevent and control NCDs rely on society-wide changes,” continues the Framework, “reflecting the interconnected nature of communities. Multisectoral national NCD plans, for example, must take the systems approach to address underlying social, cultural, behavioural and environmental factors that influence NCDs.”
The Regional Action Framework contains five objectives:
- Strengthen the mechanism to collect and use data and information for planning, monitoring progress, and evaluating policies and programmes;
- Develop policies that go beyond the health sector to enable health-promoting environments and address social determinants of health at national and subnational levels;
- Screen the population for major NCDs;
- Strengthen primary health care to provide people-centred NCD management;
- Empower patients for self-management and adherence, through health promotion, prevention and individualized data.