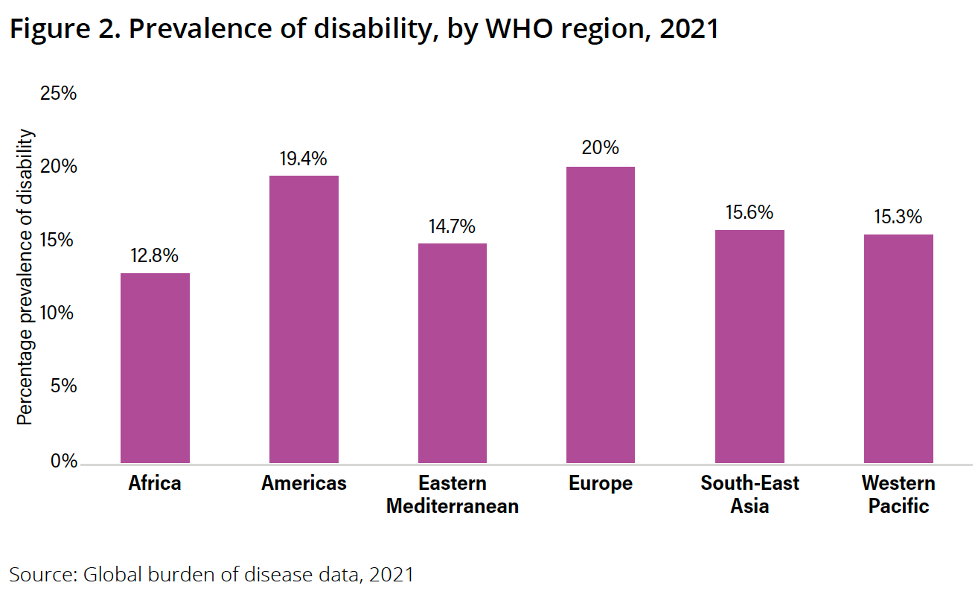
Health equity, including care for NCDs, eludes people living with disabilities

The number of people globally living with disabilities continues to grow but their ability to access healthcare, including prevention and treatment for noncommunicable diseases (NCDs) has not greatly improved in the past decade, says a new World Health Organization (WHO) report.
“Persons with disabilities continue to experience a wide range of health inequities. Contributing factors to these inequities remain unchanged during the past decade, and many persons with disabilities continue to die prematurely, have poorer health, and experience more functioning limitations as a result,” says the Global report on health equity for persons with disabilities.
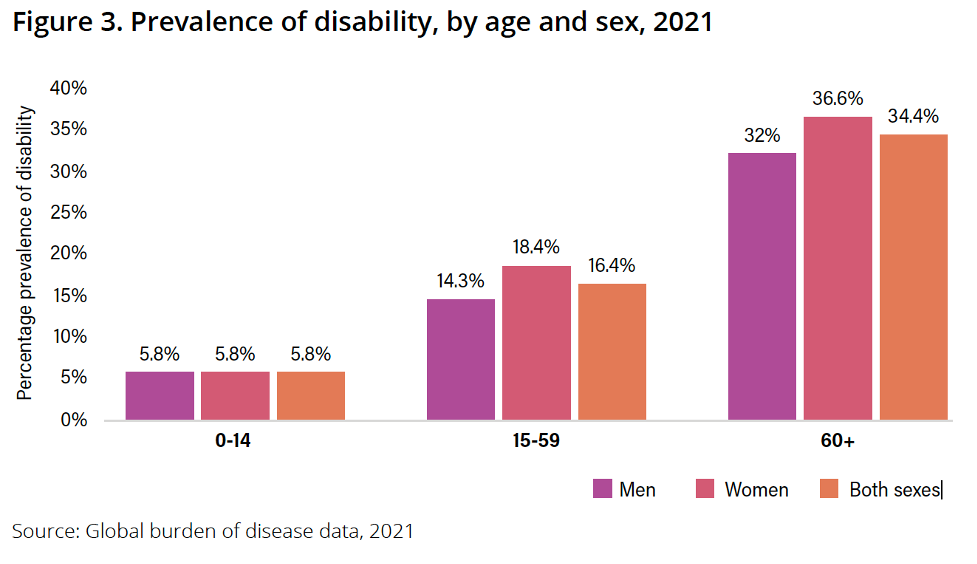
About 1.3 billion people worldwide live with a disability and that figure will keep rising, adds the document, which takes pains to stress the difference between having a health condition and living with a disability. “For example, depression, cerebral palsy or having a retinopathy are not disabilities: they are health conditions which contribute to disability if the surrounding environment negatively impacts the person’s life. A person with disability can be a child with blindness who cannot attend school because of a lack of vision assistive products and educational materials that are not adapted to their needs.”
In the report’s foreword, WHO Director-General Dr. Tedros Adhanom Ghebreyesus points out that people living with disabilities “die earlier, they have poorer health and functioning, and they are more affected by health emergencies than the general population Doing nothing to address these health inequities for persons with disabilities means denying the realization of the universal right to the highest attainable standard of health.”
Enshrined in the WHO constitution, that right is “inherent, universal, and inalienable, and is enshrined in international law through human rights treaties, and in domestic legal frameworks including national constitutions,” the report adds.
Yet, that guarantee is not always reflected in reality, despite huge returns from investments in healthcare for persons living with disabilities. Research has found that interventions for preventing NCDs, such as supplement and nutrition programmes, reach 20 percent fewer young adults with disabilities compared to the general population. In some countries, the gap in surgical interventions for cardiovascular disease between people living with disabilities and others can reach 45 percent, says the report.
But even if the average costs of interventions, with 95 percent coverage, rise by 10 percent if they are delivered in a sustained disability-inclusive way, the returns are great, the report argues. For example, implementing cancer care, with a 10 percent increase in costs, could bring an economic and societal return of nearly USD9 for every USD1 spent. The return reaches nearly USD10 per USD1 spent in disability-inclusive NCD prevention and care, assuming a 10 percent rise in costs, adds the report, which is a follow-up to the 2011 World Report on Disability.
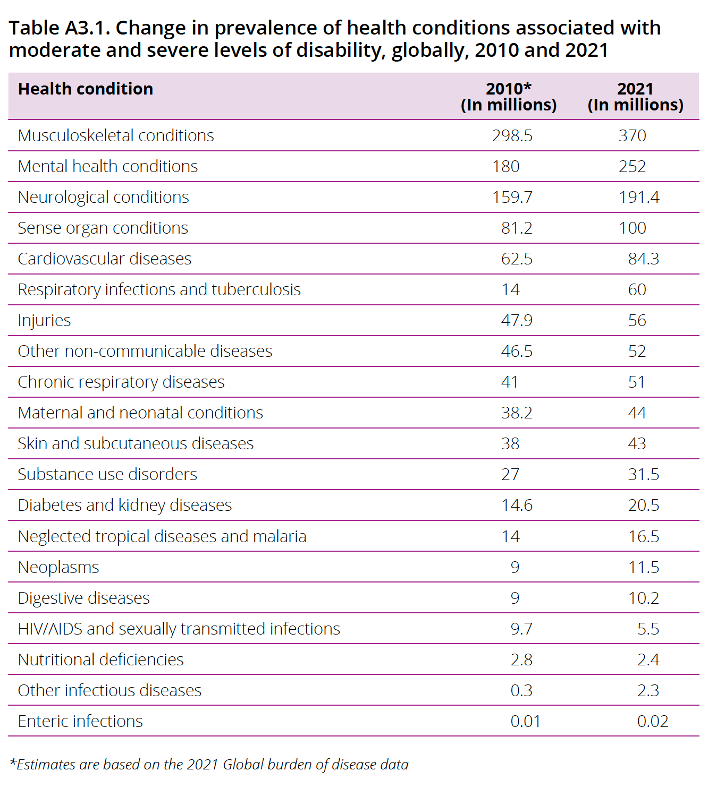
The 2022 global report notes that “disability is strongly linked with NCDs. Persons with disabilities are more vulnerable to NCDs, often because of exclusion from health-care services or other unjust factors, and… the health condition underlying a disability is frequently a NCD. In addition, people living with NCDs may develop secondary impairments, which can cause restrictions in activity and participation when supportive personal and environmental factors are not in place.
The COVID‑19 pandemic, the report adds, revealed the disadvantages that people with disabilities face within and beyond the health sector, and the need for urgent action.
At the root of health inequities are unfair conditions that affect persons with disabilities more than others. They are tied to:
- Structural factors: the socioeconomic and political context and the mechanisms that generate social stratification in societies;
- Social determinants of health: the conditions in which people are born, grow, live, work and age;
- Risk factors: the factors associated with NCDs, including tobacco use, diet, alcohol consumption and amount of exercise; and environmental factors such as air pollution. The increased exposure to these risk factors for persons with disabilities is due largely to public health interventions that are not inclusive.
In response, the WHO say the main aim of the report is to make health equity for persons with disabilities a global health priority. The document’s specific objectives are to:
- Bring health equity for persons with disability to the attention of decision-makers in the health sector;
- Document evidence on health inequities and country experiences on approaches to advance health equity in the context of disability;
- Make recommendations that stimulate action within countries.
The report recommends 40 disability-targeted actions that governments can take in 10 strategic areas of health system strengthening, noting that each country will design its approach based on its unique context. Regardless, adds the global report, certain principles “should be followed by all health sector partners irrespective of which of the specific actions… they are implementing.” These principles are:
- Include health equity for persons with disabilities at the centre of any health sector action;
- Ensure empowerment and meaningful participation of persons with disabilities and their representative organisations when implementing any health sector action;
- Monitor and evaluate the extent to which health sector actions are leading to health equity for persons with disabilities.