More of the right investment needed to address NCD funding gap—report

A new report finds—unsurprisingly—that current funding for prevention, treatment and management of noncommunicable diseases (NCDs) is grossly inadequate. But simply providing more money via the same channels is not the solution, it points out.
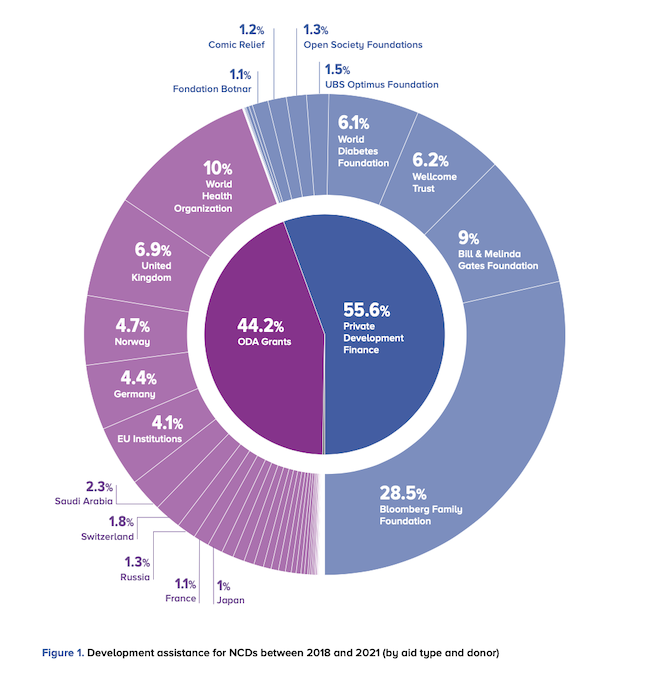
Just 1-2% of total development assistance for health (DAH) has been dedicated to NCDs over the past 20-30 years, more than half of it (55.6%) from private funding sources, finds the analysis, Tracking NCD funding flows: Urgent calls and global solutions. From 2018 to 2021 that figure might be as low as 0.8%, adds the report, led by the Global Alliance for Tobacco Control and supported by NCD Alliance.
The report was published ahead of the Second global dialogue on sustainable financing for NCDs and mental health, organized by the World Health Organization and World Bank, and scheduled for Washington, DC, 18–20 June.
NCDs are the leading cause of mortality and morbidity worldwide. Among them, cardiovascular disease, cancer, diabetes, chronic respiratory diseases, and mental health and neurological conditions account for nearly three quarters of deaths worldwide, notes the report. Today, 1.7 billion people live with NCDs, and about 86% of premature deaths and 77% of all NCD deaths occur in low-and-middle income countries (LMICs).
$18 billion needed for LMICs, 2023-2030
In 2022, the Lancet journal estimated that implementing the most cost-effective packages to address NCDs would cost an extra $18 billion per year over 2023-2030 in LMICs, but that many of them would struggle to raise money domestically and would need international assistance.
Analysing the Creditor Reporting System of the Development Assistance Committee of the Organization for Economic Cooperation and Development (OECD), the authors found that direct development financing for NCD programmes rose from 0.06% of total development assistance in 2018 to 0.11% in 2021. That is equivalent to an average of $315 million annually.
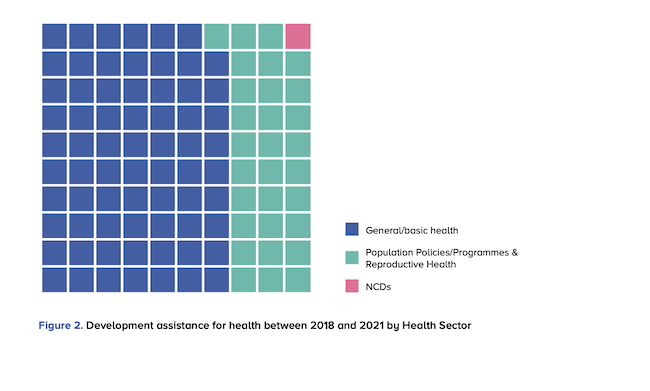
Meanwhile, funding flows to general health programmes, including infectious disease control, and to population policies/programmes, including reproductive health, made up 68.7% and 30.5% of total health-related development spending, found the report. That equals $105.3 billion and $46.8 billion respectively.
Within the NCD umbrella, tobacco control received 0.3% of total DAH, while funding for control of the use of alcohol and drugs received close to zero between the years 2018 and 2021.
‘Pooled funds for UHC’
Multi-stakeholder coordination will be required to effectively address the funding gap, advises the report. Efforts “may include, and are not limited to developing pooled funds for Universal Health Coverage (UHC) with a focus on preventing, treating, and managing NCDs.”
The authors caution that current reliance on philanthropy as the source of more than half of NCD-related DAH is concerning, since philanthropy is more vulnerable to shifts in funding priorities. By contrast, spending classified under ODA must have “economic development and welfare of developing countries as its main objective”. NCDs reduce productivity and human capital while increasing healthcare costs, making them a great threat to nations’ economic development and welfare.
“The financial burden of NCDs on households and governments creates a major barrier to poverty alleviation, a major feature of the Sustainable Development Goals,” finds the report. It recommends:
- More ODA = NCD prevention: Official development assistance (ODA) for NCD prevention should increase, and such spending should support economic development and welfare in developing countries.
- Mobilise resources domestically: To ensure sustainable funding for NCD programmes, a mix of resources, including ODA and resources mobilised domestically, is essential. “Increasing taxes on tobacco and alcohol products can be a highly cost-effective way to lower consumption and generate revenue for health system improvements.”
- More and better data: There is a critical need to invest in improved data collection and research to inform public health policies and interventions tailored to country-specific needs in LMICs. Adding more indicators for NCDs within the OECD database and other health initiatives could help improve reporting and track the impacts of NCD investments.
- Countering commercial determinants of health: Commercial determinants, such as the actions of unhealthy commodity industries (e.g., makers of tobacco, alcohol, and unhealthy foods), shape consumer environments and increase the likelihood of NCDs. This underscores the need for integrated action throughout society to influence health positively.